News
Arthritis: Updating our understanding of causes and treatment
Date posted: 5/17/2024
Last updated: 5/17/2024
Table of Contents

Today, according to the Centers for Disease Control (CDC), 1 in 5 American adults — or 53 million people — live with doctor-diagnosed arthritis. And many more have joint pain but haven’t been diagnosed yet. While there are different types of arthritis, including psoriatic arthritis, rheumatoid arthritis, and osteoarthritis, the latter is the most common. It affects 32.5 million adults.
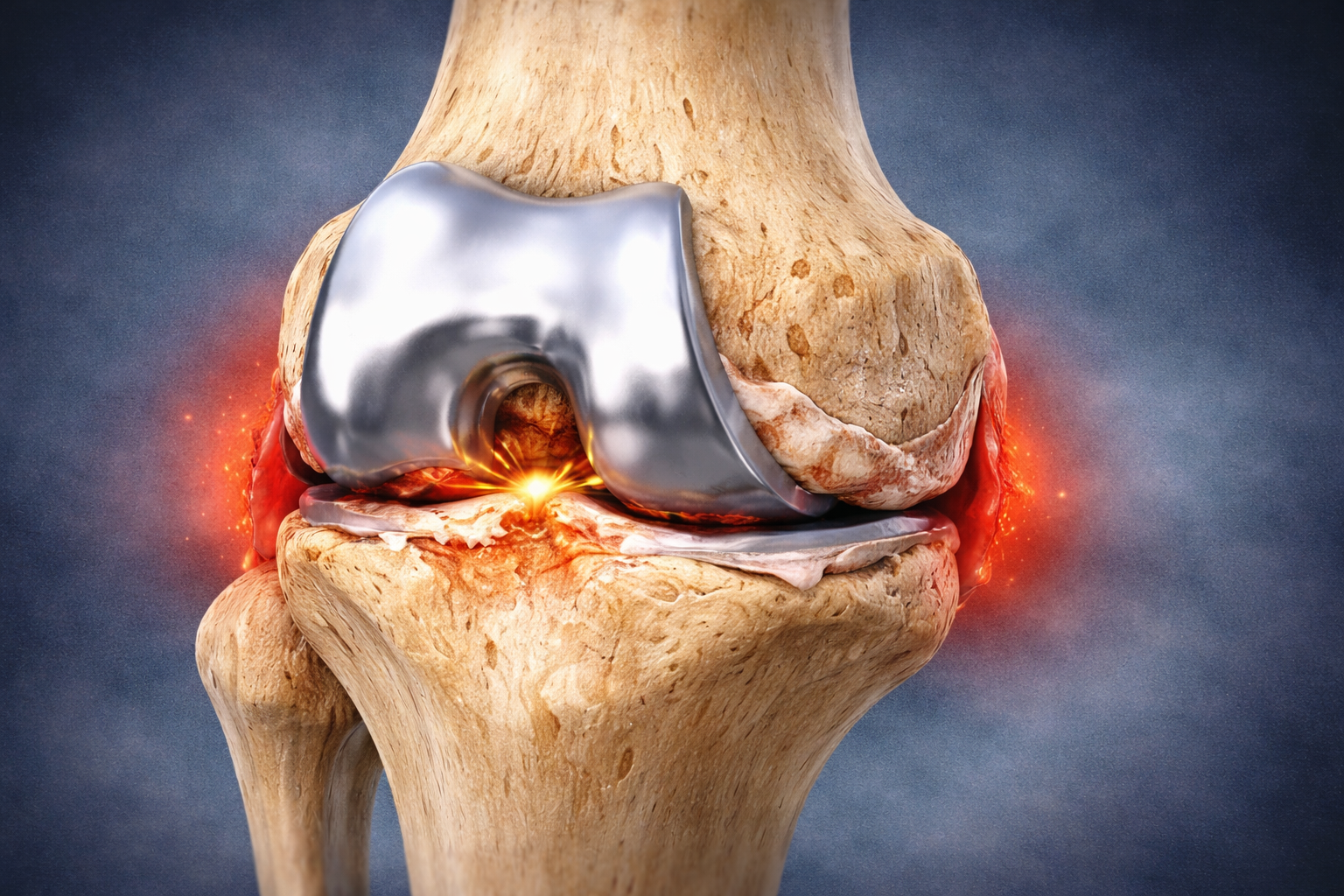
In a patient with osteoarthritis, the protective membrane between the joints (cartilage), begins to wear down. Over time, wear and tear can trigger painful inflammation which erodes the cartilage and causes structural changes in the joint. A patient may end up with no cartilage at all. Doctors today have a wide variety of conservative treatments to offer patients in the early or mid stages of arthritis and new surgical techniques including minimally invasive/outpatient joint replacement for later-stage arthritis.
We asked Midwest Orthopaedics at RUSH joint replacement surgeons some of the questions they are most frequently asked by their patients with arthritis:
Are joint replacement patients getting younger?
“I would say that patients are presenting with arthritis at younger and younger ages as a result of active lifestyles and sports-related injuries. With their desire to return to those active lifestyles, joint replacement provides an excellent option for young people with arthritis. We routinely see people return to all the activities they enjoyed before they had arthritis in their hip or knee.”
– Tad Gerlinger, MD.
Can I delay or prevent the onset of osteoarthritis?
“It's important to keep moving and stay in good shape so you're not putting extra stress on your joints. You want to keep a healthy BMI (18.5 – 24.9%). Some good ways to do that are performing low-impact activities like walking, dancing, cycling, swimming, or yoga.
Beware of overdoing it with high-impact activities like running, skiing, and gymnastics. Sports like these are a double-edged sword. They can keep you fit, but they can also put stress on your joints, so try to be mindful when practicing these activities. Listen to your body and don't overdo it!
A healthy diet is — of course — beneficial for your health all around, but it also makes a difference in joint health. As much as possible, avoid fatty foods, simple sugars or carbohydrates, and excessive salt. Eating those things can contribute to swollen, achy joints. Instead, reach for fruits and vegetables, healthy fats like olive oil and nuts, whole grains, and fish. These foods are thought to reduce inflammation and help with joint pain.
If you have joint pain that doesn’t subside on its own after a day or two, interferes with everyday life, or is steadily getting worse, it's best to talk to your doctor sooner rather than later. There is so much that can be done depending on the stage of your arthritis. Be on the lookout for swollen, red, tender, or warm joints. Your doctor can do X-rays, MRIs, or nerve tests to evaluate and collaborate with you to figure out the best path for you.
– Denis Nam, MD
Are over-the-counter arthritis relief products helpful?
“There are a lot of products on the market including various supplements and over-the-counter remedies that are widely advertised and sold to consumers and patients with hip and knee arthritis as potential cures or options for symptomatic relief. We get frequent questions from our patients regarding the efficacy of these options in managing their joint pain, swelling, and stiffness from arthritis and potentially delaying surgery, including joint replacement. It is often helpful for our patients to discuss these options with us and whether there may be a potential clinical benefit based on existing scientific evidence to support their use.”
– Omar Behery, MD
Is joint replacement the best ‘fix’ for debilitating arthritis?
“Yes, joint replacement remains the primary fix for end-stage osteoarthritis. There are a number of conservative treatment options prior to pursuing surgery that may not cure the problem but can make the symptoms more manageable. These include physical therapy, oral anti-inflammatory medications, and injections.”
– Denis Nam, MD
How do my diet and exercise affect my chances of getting arthritis?
“Arthritis progresses in different ways. It’s a combination of genetics and daily activity. For instance, someone with great genetics may be able to run and jump play professional sports and be highly active, and never develop arthritis. Others with poor genetics may just go about their daily activities and develop arthritis in their early 50’s or 60’s. The best things we can control are an anti-inflammatory diet, regular activity, and avoiding injury. Cycling, running, and playing sports, all keep the joints moving and lubricated.
Keeping a full range of motion in your joints is also key. Our society is such a sitting society. We go from our beds to cars to office chairs to the couch. Consequently, our hips don’t get a full range of motion. Other ‘floor sitting’ or ‘squatting’ cultures around the world have much less hip arthritis because they are using that joint’s full range of motion.
Another way that we can avoid early-onset arthritis is by reducing our daily sugar intake. This helps our metabolism for all parts of the body. Keeping weight down is critical. For every pound of weight, our knees feel four times the amount of force. I call it the “4 for 1” sale in our bodies. Even joint replacement patients who eat high protein and low sugar have excellent outcomes following surgery and live active, healthy lives.”
– Vasili Karas, MD